Visiting Hours and Policies

At Memorial, we strive to provide a positive patient experience and recognize the important role visitors play in the healing process. As part of BJC HealthCare, we follow a standard visitor policy to ensure a consistent experience across BJC’s 14 hospitals, multiple health service organizations and 100+ doctors’ offices. To ensure the safety of our patients, visitors and staff, some exceptions may apply.
Visiting hours are from 9 a.m. to 9 p.m. daily.
|
Area/Dept
|
Total Number of Visitors Permitted |
Visiting Hours
|
|
Emergency Department (ED) |
|
|
|
Inpatient
|
|
|
|
ICU |
|
|
|
Labor and Delivery |
|
|
|
Post-Partum |
|
|
|
Outpatient Surgery or Procedure |
|
|
|
Clinic Visits |
|
|
|
Outpatient Visits |
|
|
After Normal Visiting Hours
Safety and Security gives passes to visitors who stay after normal visiting hours. These visitors might be staying because the patient is not doing well. Only one visitor per patient may stay in the patient’s room (if in a private room) after normal visiting hours. Visitors cannot stay overnight in a semi-private room. If you are in a semi-private room, we ask that you and your visitors respect your roommate’s need for quiet and privacy.
Visitor Conduct
- Visitors should not sit on patient beds.
- Children must be with an adult at all times.
- Children under age 6 can visit if the nursing staff approves.
- If you are ill, please do not visit.
Zero Tolerance Rule
Memorial Hospitals have a zero tolerance rule. Verbal aggression will not be tolerated. Physical assault will be reported to law enforcement. No member of our staff should EVER fear for their safety while performing their work of helping the community.
No Smoking
In compliance with the Smoke Free Illinois Act and to promote health and wellness in the community, Memorial Hospital, Memorial Care Center, its diagnostic and physical therapy centers, and its medical office centers are tobacco free. Tobacco use of any kind is not permitted on any of Memorial’s properties.
The Smoking Policy also applies to the use of electronic cigarettes. The use of electronic cigarettes and vaping devices is prohibited wherever smoking is prohibited on any of Memorial’s properties.
Smoking cessation resources are available. For more information about the risk of smoking and how to quit, ask your nursing staff, or call the American Lung Association at 1-800-586-4872.
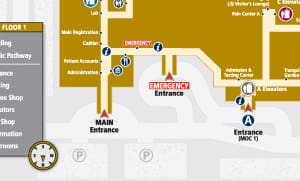
Finding Your Way Around
Looking for a specific department at Memorial Hospital Shiloh?
Online Gift Shop
Order flowers, candy, and more conveniently online! It only takes a minute to make someone’s day.